Can I Get Social Security Disability Benefits for Ischemic Heart Disease?
- How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Ischemic Heart Disease?
- About Ischemic Heart Disease and Disability
- Winning Social Security Disability Benefits for Ischemic Heart Disease by Meeting a Listing
- Residual Functional Capacity Assessment for Ischemic Heart Disease
- Getting Your Doctor’s Medical Opinion About What You Can Still Do
How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Ischemic Heart Disease?
If you have ischemic heart disease, Social Security disability benefits may be available to you. To determine whether you are disabled by your ischemic heart disease, the Social Security Administration considers whether your heart disease is severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process. See Winning Social Security Disability Benefits for Ischemic Heart Disease by Meeting a Listing. If you meet or equal a listing because of ischemic heart disease, you are considered disabled.
If your ischemic heart disease is not severe enough to equal or meet a listing, the Social Security Administration must assess your residual functional capacity (RFC) (the work you can still do, despite your heart disease), to determine whether you qualify for disability benefits at Step 4 and Step 5 of the Sequential Evaluation Process. See Residual Functional Capacity Assessment for Ischemic Heart Disease.
About Ischemic Heart Disease and Disability
What Is Ischemic Heart Disease?
Ischemic heart disease (IHD) is a major medical problem disabling and killing millions of people in the U.S. yearly, and therefore a frequent basis for allegations of disability. Heredity plays an important role, but so does lifestyle. Many IHD deaths are preventable and associated with poor control of hypertension and diabetes mellitus, smoking, lack of exercise, obesity, and poor diet resulting in elevated blood lipids (fats such as cholesterol).
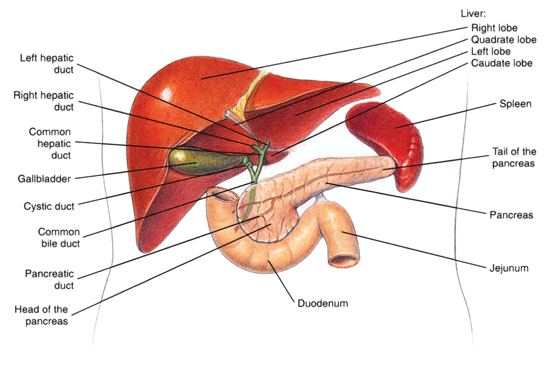
Ischemia means that the heart (or other body tissue) is not receiving enough oxygen to function normally. The oxygen demands of the heart change with heart rate (see Figure 1 below). So increased heart rates require increased blood flow to the heart to deliver the oxygen and glucose needed for the extra work. Ischemia not present at rest may appear when the heart rate increases, and this is the basis for cardiac stress testing. See Cardiac Stress Testing.

Figure 1: The path of oxygenated and unoxygenated blood in the heart during contraction.
Causes of Ischemic Heart Disease
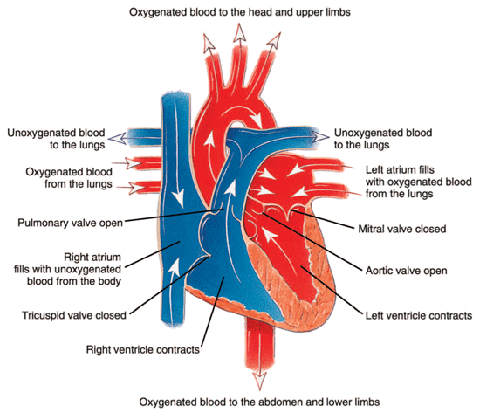
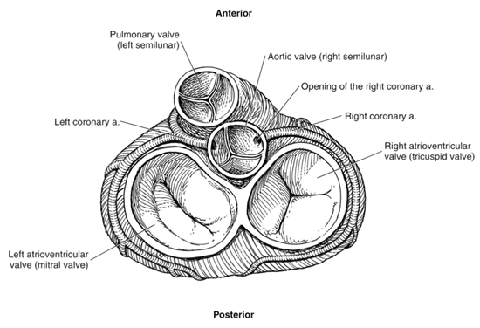
Most IHD results from obstruction of the coronary arteries that supply the myocardium (heart muscle) with blood. This condition is known as coronary artery disease (CAD). Other cardiac abnormalities can also cause myocardial ischemia. The underlying mechanism is still the same: restriction of blood flow to the myocardium. For example, marked narrowing of the aortic valve (aortic stenosis) (see Figure 2 below) can cause angina (chest pain) because the coronary arteries originate right above the valve (see Figure 3 below) and may not receive sufficient blood flow to supply the heart. However, the great majority of claimants have myocardial ischemia because of CAD.

Figure 2: Closed heart valves.

Figure 3: Anterior view of the heart, including main arteries.
How Severe Does Coronary Artery Disease Have to Be to Produce Ischemia?
Blood flow to the myocardium served by a particular coronary artery is not significantly decreased until a lesion blocks about 70% of the diameter of the artery. It is frequently possible for a person to be comfortable at rest with a 90% blockage in a large epicardial artery.
Lesions of less than 50% are generally considered to not be significant CAD, because the heart will still be able to obtain sufficient blood flow both at rest and with exercise. However, this conclusion must be made in context of all of the medical evidence. Long segments of obstruction rather than discrete lesions, involvement of the left main coronary artery, or involvement of multiple arteries could cause significant ischemia with blockages as low as 50%.
Detecting Ischemia
Ischemia can be indicated by:
- Electrocardiograms (ECGs, ECGs);
- Imaging studies that show the movement of the cardiac ventricular walls;
- Imaging studies that show relative blood flow within the heart muscle; and
- Imaging studies that measure amounts of blood moved by the heart’s ventricles.
Cardiac Stress Testing
Cardiac stress testing raises heart rate to determine:
1) Whether ischemia can be induced,
2) The level of exertion producing ischemia, and
3) The severity and location of the ischemia.
Cardiac stress testing is also used to determine the exercise capacity of individuals in regard to physical conditioning, but the Social Security Administration never purchases testing for that purpose alone.
The only type of cardiac stress testing mentioned by the Social Security Administration is exercise stress testing, in which physical exertion is used to raise the patient’s heart rate.
In exercise stress testing, your baseline ECG is obtained. Then you begin with a low level of exercise, either by walking on a treadmill, or pedaling a stationary bicycle. Every two to three minutes, the level of exertion is increased. At each stage of exercise, your pulse, blood pressure and ECG are monitored are recorded, along with any symptoms you may be experiencing.
The exertion level is gradually increased every 2 to 3 minutes until you cannot keep up any longer, or until your symptoms (chest pain, shortness of breath, or lightheadedness) prevent further exercise, or until changes on your ECG indicate a cardiac problem.
There are other means of raising heart rate for testing purposes, such as pharmacologic stress testing in which drugs are used to raise the heart rate. Pharmacologic stress testing can be used with patients who, for some reason, cannot perform exercise stress testing.
Both exercise testing and pharmacologic testing can be used in conjunction with various types of imaging studies of the heart’s response to increased heart rate—such as radionuclide scans or echocardiograms that are done at the same time.
Left Ventricular Ejection Fraction
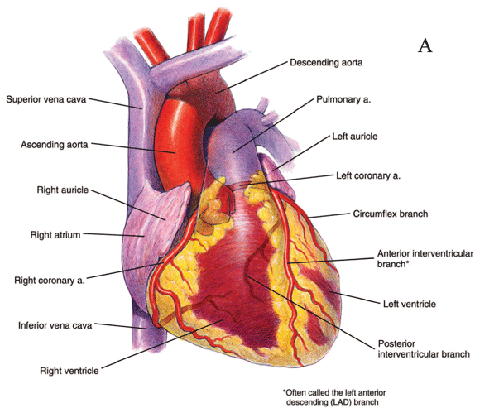
The most important performance test for blood moved by cardiac ventricles (see Figure 4 below) is the percentage of blood pumped out of the left ventricle (LV) with each beat—the left ventricular ejection fraction (LVEF). The left ventricle is of major interest, because it pumps blood into the systemic circulation that supplies the tissues of the body and is the major site of damage by ischemic heart disease, such as heart attacks.

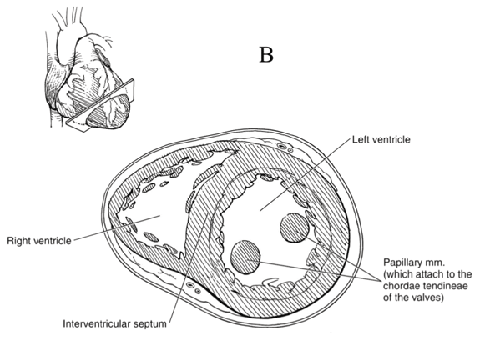
Figure 4: Cross-section of the ventricles of the heart, which are important to blood movement.
The LVEF is normally about 55-65%, and is not usually considered abnormal unless it falls under 50%.
Angina Pectoris and Ischemic Heart Disease
What is Angina Pectoris?
When the myocardium receives inadequate blood flow, sensory nerve fibers (cardiac afferents) from the heart to the brain carry impulses for pain known as angina pectoris. The Social Security Administration also refers to angina as “chest discomfort of myocardial ischemic origin.”
In a significant number of people with myocardial ischemia, the pain activation system is defective for no obvious reason. These people have no warning when blood flow to the heart is inadequate and they are at particular risk for sudden death. Without warning pain, such individuals may continue to exercise after the onset of ischemia. Ischemic heart muscle is electrically unstable, so that it carries an increased risk of a lethal arrhythmia.
Angina and Disability
Angina is relevant to disability determination. To meet the listing for ischemic heart disease, you must have symptoms due to myocardial ischemia. See Winning Social Security Disability Benefits for Ischemic Heart Disease by Meeting a Listing. Angina is one such symptom. See Symptoms Due to Myocardial Ischemia.
Angina is also relevant to disability determination because chest pain limits exertion. In disability adjudication, the Social Security Administration frequently must evaluate the status of claimants after a myocardial infarction. See Heart Attacks (Myocardial Infarctions or MIs).
Many allege chest pain that may or may not be of cardiac origin.
However, there are too many unknown variables, conflicting descriptions, and other confounding factors to use the absence or presence of chest pain—even classic, angina-compatible chest pain—as controlling either treatment or disability decision-making.
Objective Data Are Necessary for Diagnosis of Angina
Objective data (test results) supporting the angina diagnosis are necessary. A diagnosis of angina based on a patient’s description alone is not reliable. Many claimants who describe chest pain that could be angina based on the description they provide (angina-compatible chest pain), turn out to have nothing wrong with their hearts after thorough examination.
A number of medical conditions can cause chest pain closely resembling angina. Esophageal spasm, for example, can feel just like angina—even be relieved with drugs used to treat angina—except for one thing: the absence of relation to exertion. A good history of chest pain that covers the possible non-cardiac types of pain requires a careful approach and professional medical training. Shortness of breath may occur with angina, but shortness of breath alone is not angina.
The Social Security Administration must obtain cardiac exercise testing on claimants with angina-compatible chest pain when there is no other means of allowance and there is no contraindication to such testing. See Cardiac Stress Testing.
Characteristics of Angina
Angina is described in terms of:
- Location,
- Quality,
- Precipitating causes,
- Duration, and
- Mode of relief.
The general characteristics of these factors are as follows:
Location – Central Chest (Substernal)
Angina pain sometimes radiates down one or both arms or up into the neck or jaw. Angina is much less likely if the pain is only outside of the central chest area, such as in the jaw alone, or abdomen. Pain in a small area on the side of the chest is probably not angina. The more unusual the location of pain, the less likely that angina is actually the cause. However, if other characteristics fit the diagnosis of angina then it should be accepted despite an atypical location—especially if there is objective evidence of significant ischemic heart disease. In fact, the Social Security Administration is willing to accept atypical locations—even pain isolated to a hand, jaw, or neck—if everything else fits the angina diagnosis.
Quality – Dull, Aching, Squeezing, Heavy
Most claimants describe their pain as “sharp.” For some reason, this is the first word that enters the mind for many people when asked the quality of a pain. Therefore, a diagnosis of angina should not be discarded because a claimant uses the word “sharp.” Less-educated claimants are particularly likely to use words for the quality of chest pain that actually do not describe what they are experiencing. Because of the subjective nature of “quality”—what something feels like—the Social Security Administration adjudicator should only reject the characteristic if the quality described is something that is never associated with angina.
Rhythmic pain is never angina. Rhythmic pain is something that rapidly varies in intensity, especially stabbing, jabbing and poking sensations that quickly come and go (also see the discussion of Duration below). It is important for the interviewer to carefully communicate with the patient in this regard to make sure that there is mutual understanding of the meaning. For example, sticking or “pins-and-needles” sensations are also not compatible with angina.
Precipitating Causes – Exertion, Emotion
Exertion and emotion (excitement, anxiety, fear) raise heart rate, which can induce cardiac ischemia and the onset of ischemic chest pain—angina. Chest pain that always occurs with particular activities, such as walking a certain distance or climbing a certain number of stairs is characteristic of angina.
Chest pain with exertion does not always indicate angina. Chest pain that occurs randomly, sometimes during exertion and sometimes during rest, does not suggest ischemia since the cause-and-effect element is missing.
Chest pain associated with emotion, but occurring at rest, could be angina. On the other hand, chest pain that occurs only with emotion and not with exertion is suspect for being of non-cardiac origin.
Although there should be a general cause and effect relationship between angina and exertion or emotion, that does not mean that angina will always occur at a specific level of exertion since multiple factors (e.g., emotional state, physical health, drugs, temperature) can influence it. The absence of chest pain during exercise testing is not sufficient, in itself, to rule out ischemic heart disease. Nor is it sufficient to eliminate a claimant’s subjective report of chest pain during activities of daily living from consideration. Also, some individuals may show evidence of ischemia during stress testing, but have no pain.
Ischemia and reported symptoms are not predictably associated. Similarly, ischemia at any particular level of exercise cannot be closely predicted on the basis of the underlying coronary artery lesions.
The important piece of information needed for either treatment or disability determination is objective, exercise-induced ischemia.
Vasospastic Angina
There is an important exception to the relationship between exertion and ischemic cardiac chest pain: vasospastic angina (variant angina) occurs when a coronary artery narrows in a particular location, thereby decreasing blood flow to heart muscle past the point of narrowing. The word “vasospastic” means that the narrowing is temporary, and usually results from some irritative focus that causes the smooth muscle inside the coronary artery to constrict at a specific place. The irritative focus is something that triggers the muscle spasm and that is often the fibro-fatty, sometimes calcified, plaque of coronary artery disease.
Drugs like cocaine are particularly likely to induce coronary artery spasm. In fact, cocaine can cause such severe constriction that blood flow is completely cut off to an area of the heart, with a resultant heart attack in a young person who would otherwise not have such an event. The risk is probably even greater for a middle-aged person who already has an irritative focus like a fatty lesion in a coronary artery and then also takes cocaine.
Angina in the Resting State
It is possible to have cardiac ischemia so severe that angina occurs in the resting state. But these people are so ill that they have been evaluated for heart disease by their treating physicians and severe abnormalities have been documented. Angina occurring in the resting state either results in medical treatment or death. No one with angina at rest is going to be in that state very long without medical care. Furthermore, angina in such cases will still be characteristically precipitated by exertion and worsened by exertion, so that important cause-and-effect relationship is still intact.
Duration
Typical angina lasts only a couple of minutes after the precipitating cause is stopped. It is quite common for claimants to say that their chest pain lasts for hours at a time on a regular basis. This is not anginal chest pain. Chest pain lasting for hours is more compatible with a heart attack than angina. Even if a person has particularly severe and worsening angina—a condition known as unstable angina—there is no way such prolonged angina could be occurring on a regular basis, because the individual would be dead or in a hospital.
Attempting to continue exertion with angina will cause further worsening until the person stops the inducing activity, which will happen quickly after the onset of pain; no one ignores angina.
Chest pain lasting less than a minute is usually not angina. Chest pain lasting less than 10 seconds or more than 30 minutes would be considered non-anginal by most cardiologists. In the unusual cases in which 30 minute durations are caused by ischemic heart disease, they are more characteristic of unstable angina, than typical angina. Unstable angina is a serious condition and not something a person has very long without coming under medical care. Nevertheless, the Social Security Administration is usually generously flexible in this regard. If all of information is supportive of the diagnosis, durations of up to 30 minutes will generally be accepted in disability determination as angina, rather than requiring a more realistic 3 to 5 minutes of duration. Perhaps this is because the Social Security Administration realizes that many people are poor at estimating the time their chest pain lasts. Of course, the optimum situation is one in which patients have actually measured the duration of pain after cessation of the precipitating cause, but claimants usually have not done so.
Relief of Angina
Angina caused by exertion is relieved by rest; emotionally induced angina is relieved by lessened emotional arousal.
A number of long-acting drugs improve cardiac ischemia and decrease the over-all frequency and severity of anginal attacks. For example, beta-blocker drugs like propranolol will keep the exertional and emotional heart rate down. Long-acting nitrates will help keep coronary arteries widened to maximize blood flow.
Treatment of high blood pressure (HBP) will decrease the work the heart has to do and therefore improve angina.
Nitroglycerin taken as a small white tablet dissolved under the tongue (not swallowed) has long been a standard treatment for acute relief of angina by dilating coronary arteries. Nitroglycerin will typically relieve angina in 30 seconds to several minutes. Unfortunately, nitroglycerin tablets also relieve the non-cardiac pain of esophageal spasm—a common disorder—so that an improvement with nitroglycerin, which is suggestive of possible angina, is not diagnostic.
Syndrome X
Syndrome X refers to angina-compatible chest pain in people with normal epicardial coronary arteries. Around 10% to 20% of individuals with angina-compatible chest pain have normal epicardial coronaries. The dilemma is determining which ones have some true cardiac basis for such pain (Syndrome X) and which have some other physical disorder or psychiatric impairment.
Unlike classic angina (associated with ischemia from epicardial artery obstructions) and vasospastic angina (associated with ischemia from reversible epicardial artery spastic narrowing), individuals with Syndrome X have no obvious cause of ischemia to explain their chest pain symptoms. Some of these individuals have objective evidence of ischemia on exercise test ECGs, as well as on radionuclide scans for cardiac ischemia and positron emission tomographic (PET) scans.
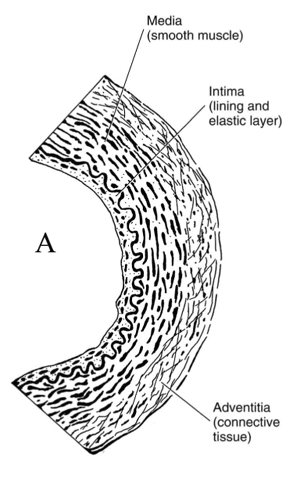
Individuals with Syndrome X are speculated by some authorities to have microvascularangina resulting from spasms in the smaller arteries (see Figure 5 below) within the heart muscle (intra-myocardial arteries), or perhaps an inability of these arteries to adapt to needed changes in blood flow. Very small coronary arteries cannot be directly visualized by coronary angiography—only the epicardial arteries and their branches.

Figure 5: The micro-structure of an artery.
Some authorities believe that ischemic dysfunction in Syndrome X occurs on a cellular level that cannot be adequately categorized without even further refinement of imaging techniques to a molecular level.
The significance of Syndrome X for disability determination is that the Social Security Administration should not ignore objective evidence for cardiac ischemia because the medical evidence shows normal coronary arteries visualized by cardiac catheterization and cardiac angiography.
Some treating physicians simply speculate that a patient has Syndrome X without documenting objective evidence of ischemia. The Social Security Administration is not obligated to consider such individuals disabled on the basis of alleged symptoms alone.
There has to be some objective cardiac basis for chest pain symptoms before allowance under the listing is possible, but that evidence may take several forms and the normality of one form of evidence—such as coronary angiography of the large epicardial coronary arteries—is not sufficient basis to rule out ischemia demonstrated by other means. See Winning Social Security Disability Benefits for Ischemic Heart Disease by Meeting a Listing.
Heart Attacks (Myocardial Infarctions or MIs)
Heart attacks (myocardial infarctions, MI) result when blood flow to a part of the myocardium decreases so much that the tissue dies. Unlike ischemic tissue, infarcted tissue cannot recover. MIs may be of any size, from one so small that there is no significant long-term impairment to events involving so much heart muscle that the heart cannot pump enough blood to maintain life.
MIs killing half or more of the myocardium are not compatible with life. Fortunately, most heart attacks are much smaller.
Although MIs can affect the right ventricle of the heart, they most often occur in and damage the pumping ability of the left ventricle. If severe enough, the left ventricular ejection fraction will decrease.
In some individuals, heart attacks are so massive that cardiogenic shock develops, a life-threatening condition in which the heart’s function is not good enough to maintain blood flow. A heart attack resulting in cardiogenic shock should cause a Social Security Administration adjudicator to suspect a large heart attack occurred.
In the past, if a heart attack appeared in a claimant’s medical records, it was considered significant. However, with the development of supersensitive biochemical tests for cardiac muscle damage, even very small amounts of heart damage (as little as 1 gram of heart muscle) will give a positive test result. This means that a technical diagnosis of a MI provides little information about the amount of heart damage. The impairment could range from none to marked. This has become a real problem because of patient self-perception and the effect on employability and health insurance.
Heart attacks do not necessarily result in disability, or limitation to light or sedentary work, or the need for prolonged recuperation and rehabilitation. The Social Security Administration assumes a 3 month interval for recovery from an MI before making a disability determination. It is now known that small heart attacks reach maximum healing in about 5 weeks, and large heart attacks in about 2 months.
The concept that all heart attacks are devastating events is not correct; each case must be evaluated on its own evidence. The very sensitive troponin cardiac enzyme tests now routinely used to diagnose heart attacks will nearly double the frequency of a diagnosis of acute MI compared to the past when less sensitive tests were available. This also means much smaller volumes of cardiac damage will be detected resulting in more diagnoses of MI, which emphasizes the need for professional medical judgment in adjudicating such claims.
Continue to Winning Social Security Disability Benefits for Ischemic Heart Disease by Meeting a Listing.